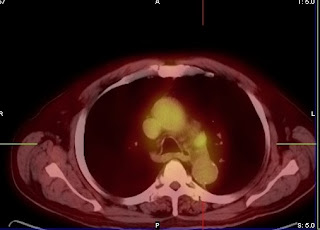
Patient is a 68 year old African American woman with a history of non-Hodgkin's lymphoma treated with chemotherapy and radiotherapy in 1980.
Symptoms now: she has type-B symptoms only - sweats at night, lost 14 pounds in the last 2 months, 7 pounds in the last 1 month. Low appetite also. There are no respiratory symptoms at all.
She also has burning feeling in the feet
She has right hilar and subcarinal adenopathy; she also has gastrohepatic and periportal adenopathy and slightly more prominent intrahepatic biliary tree dilatation with slightly more dilatation of the previously dilated common bile duct.
A surgical excision biopsy of an axillary node showed non-caseating granulomatous inflammation with no lymphoma at all.
Again her symptoms are as above - some B symptoms and a likely peripheral neuropathy (I think).
How would you approach this patient next?
Wednesday, May 28, 2008
Thursday, May 22, 2008
Update on cavitary lesion
Well, I thought this patient would have active TB. 3 AFB's were negative. Here is a CT we then got:


We bronched her and all AFB's are still negative, 6 days later. The TBBX was also negative:
minimal inflammatory cells. Bronchial mucosa and submucosal glands are unremarkable. Alveoli show few pigment laden macrophages. No evidence of granulomas or viral inclusions is seen. AFB stain is ordered, see addendum.
She is currently taking 4 drug TB therapy (after bronch)
What would you do now??


We bronched her and all AFB's are still negative, 6 days later. The TBBX was also negative:
minimal inflammatory cells. Bronchial mucosa and submucosal glands are unremarkable. Alveoli show few pigment laden macrophages. No evidence of granulomas or viral inclusions is seen. AFB stain is ordered, see addendum.
She is currently taking 4 drug TB therapy (after bronch)
What would you do now??
Thursday, May 15, 2008
What do you see?
The patient is a 59-year-old female with history of hepatitis C, currently on dual therapy with pegylated interferon and ribavirin for last 2 months presented with complaint of cough.
PAST MEDICAL HISTORY:
1. Hepatitis C, liver cirrhosis.
2. Childhood asthma.
3. History of positive PPD more than 10 years ago, which was positive, at
that time with negative chest x-ray.

PAST MEDICAL HISTORY:
1. Hepatitis C, liver cirrhosis.
2. Childhood asthma.
3. History of positive PPD more than 10 years ago, which was positive, at
that time with negative chest x-ray.

Monday, May 12, 2008
stage iiia?
Subscribe to:
Posts (Atom)