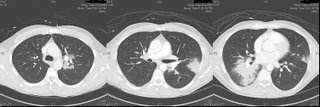
I bronched him, and it was non-diagnostic. I sent him for a surgical biopsy.
The report was read as BOOP with an microscopic sulfur granules c/w actinomycosis.
I started him on Augmentin and saw in the office in 3 weeks.
He was no better. Spiro was c/w were moderate restrictive vent defect.
So, I started him on steroids at 40 mg/day of prednisone x 3 weeks then 30 mg/day.
I saw him 4 weeks later (about 1 week into his 30 mg/day) without any clinical improvement.
His full PFT's are c/w mild obstruction with air trapping and impaired gas exchange (DL ~70% predicted). He is a smoker, and is still smoking about 1/2 ppd.
I had his biopsy reviewed by Jeff Myers at U of M (profoundly smart and helpful- wish he would have joined the faculty 5 years sooner), but he thought the original interp was correct.
Now what?
6 comments - CLICK HERE to read & add your own!:
Maybe I could beat Jeff Myers. Norcaridia can cause BOOP with sufar granules too.
HIV status ?, any CNS involvement?
Would try Bactrim.
Infection can cause BOOP-like changes. In this clinical context I agree that actinomycetes would be the likely culprit of the patient's findings. It would also explain lack of improvement from steroids. Because the treatment is long-term penicillin-G, and because (as anon pointed out) Bactrim would be indicated for nocardia, you might want to re-sample, OR you could just treat with the pcn.
How is his dentition?
He already got 3 weeks of augmentin without improvement.
Stains on the BAL for AFB were negative and fungal cultures for nocardia (now at 8 weeks) are final and negative.
Cultures/smears on the surgical biopsy are equally negative.
This guy has already had a bronch and a surgical biopsy; what are you thinking might result from additional specimens?
I think Cx sensitivity is never 100% and since there is a disconnect between the clinical impression (i.e. sulphur granules, inflammation) and response to Tx, resampling might identify an organism that was previously missed with low morbidity (from a BAL for instance).
what about doing a lobectomy
Treat with a prolonged period with abx ( PCN ) will be my choice and repeat 6 CT scan in 6 month. I would give steroids for 6 month at least before taper.
Post a Commenttest post a comment