He presented with sub-acute (a few days) onset of low-grade fevers and cough productive of scant purulent sputum. No weight loss, no hemoptysis.
PAST MEDICAL HISTORY: Chronic obstructive pulmonary disease, chronic headaches, no cardiac disease.
SOCIAL HISTORY: Significant for previous smoking history. Quit 2 years ago. No alcohol abuse, no illicit drug use. No significant occupational exposures.
ROS and FHx non-contributory.
Exam: AAOx3, in NAD. Most of exam was unremarkable except for respiratory: chest ymmetrical with good expansion bilaterally, increased AP diameter. Hyperessonant to percussion throughout. He has a very prolonged expiratory phase throughout with decreased aeration bilaterally and bilateral upper lobe rhonchi.
Chest radiograph below.
What would the DDx and what would you do next?
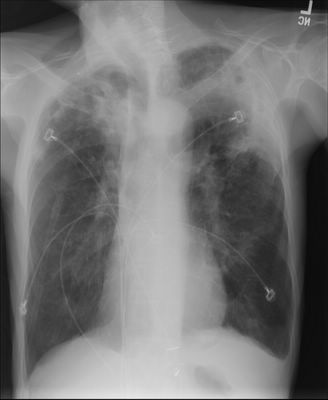

10 comments - CLICK HERE to read & add your own!:
He had an OSH CT scan, which confirmed the bullous dz but no cavities. Just the dense infiltrates seen on the CxR.
PPD was negative.
Hmm..bilateral infiltrates with what looks like pleural involvement as well, on the left upper. Alsp maybe a left pleural effusion.
1. I'm not sure if I would rest my hat on the negative PPD. Would still be concerned for TB
2. You said he has no occupational exposures so I won't go down that path, but beryllium would be a top choice otherwise, although lack of hilar adenopathy would be a bit atypical)
3. Sarcoid - it would have to be a stage 3. Also pleural involvement can definitely occur with sarcoid so his pleural stuff doesn't rule that out.
4. does he have peripheral eosinophilia? I was thinking of chronic eos. pneumonia.
5. The bullous disease could be his emphysema, but in this smoker might need to consider eosinophilic granulomatosis. His age is a bit atypicial I realize, but he is a smoker with b/l upper lobe disease and the rest of his lung zones also seem to have som ILD-like changes, also notable on the lateral. Especially with his underlying emphysema, you can still see the markings.
I would bronch and biopsy him. sending the BAL for cell count diff and the other usual stuff. Might want to check the CD1a etc etc
oh and some autoimmune stuff like ankylosisng spondylitis but you didn't give a history to indicate this.
No involvement of joint, skin, etc. to suggest collagen-vascular dz. The bullous dz was very typical of bullous emphysema with a new superimposed process.
No TB exposure. Old CxR showed the same hyperinflation but the infiltrates are fairly new.
If these upper lobe infultrates are new, than it argues against my first thought which was upper lobe fibrosis and retraction from (probably) old Tb.
Since they are new, it's much more concerning. Upper lobe-> ?sarcoid, ?EG, but neither seems likely given the history. ? Subacute HP-not a typical picture. Any nodes on the CT scan? Still could be re-activation Tb. I agree with bronch/BAL and TBBX.
Also, silicosis can look like this, although the pleural involvement would be atypical and there is no history of exposure given.
Last one---I just looked again at the lateral, and it looks like there's collapse/atalectasis of the RUL. I'd also be looking for an endobronchial lesion, which in this case would raise the possibility of a multifocal/metastatic carcinoma. But, I'm not sure I'd expect this in the absence of any mediastinal LAD.
I am officially withdrawing for consideration sarcoid, as the guy is too old. As for the silicosis, it should be nodular. Even the conglomerate silicosis should be nodular. Also, he said there was no occupational exposures.
I'm not sure if carlos's lack of response to the comments so far mean that the correct answer has not been mentioned yet, or if one of us did put the correct dx but he is just waiting for more comments???
He had come in on a Friday and was placed on resp isolation for the reasons you outlined. He was scheduled for a bronch on Monday but over the weekend his sputum smears were + for large AFB.
His PPD was negative. We started him on 4-drug TB Tx and sent him home.
On F/up he was much better with clearing infiltrates. His Cx though grew M. kansasii and no MTb.
Post a Commenttest post a comment